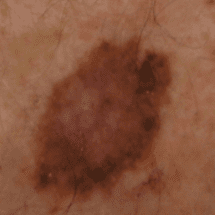
Melanoma
Malignant melanoma
Malignant melanoma is the most serious form of skin cancer arising from the pigment producing cells in the skin known as melanocytes.
Melanoma is the most common cause of skin cancer death worldwide. Unfortunately, New Zealand has the highest incidence of melanoma and Tauranga, the highest incidence within New Zealand. Chances of curing melanoma are directly related to how deep it has grown in the skin when diagnosed. The earlier it is picked up, the higher the chance of cure. If treatment is left too late, melanoma has the ability to rapidly spread throughout the body and lead to death.
Melanoma most commonly arises from a new or changing mole on the skin, although rarely can occur on the skin of the palms, the soles of the feet and even the nails.
Your specialist will discuss the best method to diagnose and treat a lesion suspicious for melanoma and discuss additional treatment or investigations that may be required if a melanoma is diagnosed.