Eczema
What is eczema?
Eczema is the common name for dermatitis and doesn’t describe a single skin condition, but a group of diseases which cause inflammation of the skin. Though still inconclusive, researchers believe the disease to be related to our immune system which causes problems in the way our skin acts as a barrier The inflammation has a huge range of presentations and accompanying symptoms associated with an equally broad range of contributing factors and suspected causes.
Who Gets Eczema?
In 2015, this troublesome skin condition was estimated to affect 245 million people worldwide. It occurs in around 20% of children and 3% of adults but can happen anytime; usually worst between the ages of two and four then improves, often disappearing altogether by the teens.
Certain occupations are more likely to cause this condition, such as farming, hairdressing, domestic and industrial cleaning, domestic duties and caregiving; exposing the skin to water, detergents, solvents, irritants, and allergens and aggravating symptoms. If you are prone to eczema, choose appropriate career options as early in the piece as possible to avoid later struggles.
Is There A Cure For Eczema?
Currently, there is no known cure for eczema. However, research is ongoing, and there are very effective treatments available.
Are There Different Types Of Eczema?
There are four main subcategories of dermatitis or eczema: Atopic, Allergic Contact, Irritant Contact, and Stasis.
What Is Atopy And How Does It Affect My Eczema?
‘Atopy’ or an ‘atopic tendency’ refers to the mostly inherited inclination of certain people to suffer a combination of asthma, eczema and hay fever in varying degrees. Atopy often runs through members of the same family. Sufferers can appear to be ‘hyper-allergic.’
How Does Eczema Look And Feel?
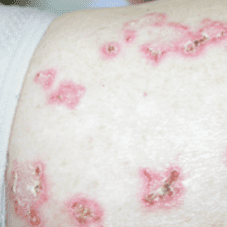
Every type of eczema has different symptoms, but the primary offender is itchy skin. Other common signs include dryness and redness of the skin, swelling, and lesions which sometimes ooze and scar. The area where symptoms arise tends to be different with all eczemas, whether on the neck, wrist, forearm, thigh or ankle. More rarely, it may appear in the genital area, such as the vulva or scrotum. Symptoms of dermatitis may be very intense, and it may come and go.
Having eczema means that you can be more susceptible to infection (boils, folliculitis, cold sores, thrush) due to reduced barrier function and subsequent breaks in dry, split skin, from scratching. Those infections can quickly become severe so treat as soon as possible.
The presence of infection, additional skin conditions, and creams applied can affect the way eczema looks and feels, as can age and ethnicity.
What Causes Eczema?
There is no single cause for eczema, believed by researchers to arise from of a complex interaction of genetic and environmental factors.
The immune system, which develops in the first six months of our lives, is thought to be the primary problem. There can be abnormalities which occur during the development period which alter how our bodies respond to infections or imbalances. With eczema, the imbalances are thought to change the way our skin acts as a barrier, causing increased permeability or absorbency of the surface which reduces its standard anti-bacterial functions. The skin becomes more susceptible to irritation from soap, contact irritants, the weather, temperature and other nonspecific triggers, which manifests with dryness, redness, itching and so on.
How Can I Be Certain I Have Eczema?
Due to the extreme complexity of this disease and its potential causes, it’s vital to seek specialised advice from reputable practitioners. Skin Centre’s team of highly qualified, skilled and experienced dermatologists are world-class, relentlessly keeping abreast of current research. You can be confident they’ll leave no stone unturned to find the best option for your specific treatment needs.
Diagnosis will be made following a comprehensive physical examination of your skin and will depend on the pattern, severity, and duration of your signs and symptoms. Also crucial will be the in-depth consultation with your dermatologist regarding your medical history; including familial, occupational, and lifestyle factors.
Are There Other Causes Of Eczema?
Additional areas of research into the cause of eczema are genetic mutations and abnormalities in skin cells. Also, certain microorganisms in particular body sites might account for the characteristic appearance of active lesions; for example, the moist elbow and knee creases.
What Are Some Common Irritants To Eczema?
Climate undoubtedly plays a significant role in the severity of eczema. Cold, damp climates can cause the disorder to become more resistant to treatment. Conversely, it’s common for patients to become itchier with redder skin when hot.
People will usually notice that certain things seem to irritate their skin with immediate stinging or itching, perhaps with a flare up. This response falls under the category of irritant contact dermatitis and is not the same as an allergy.
Examples of common irritants are:
- Frequent washing
- Washing with extremely hot water, hard water, or soap
- Harsh clothing detergents
- Coarse clothing or clothing seams
- Cosmetics and perfumes
- Certain topical creams
- Dusty environments
- Chlorine in swimming pools
Can Stress Affect Eczema?
Physical, mental or social stress has shown an increased likelihood of a flare up in your symptoms; this includes things you may not have considered such as a common cold or an underlying illness.
Eczema itself may be the source of stress due to the degree of discomfort, embarrassment and financial cost of medications and time away from work.
Are Allergies Linked To Eczema?
The nature of a person with atopic tendencies has caused a lot of misunderstanding regarding the link between eczema and allergies, especially food allergies. While it’s true that atopic patients are likely to have allergies to food or environmental factors such as grass, cat dander, and dust mites, these allergies are often independently, so it’s not possible to conclude a definite relationship between the two. Current research indicates that the skin barrier defects which occur with eczema alter immune function and so can induce food allergy secondarily.
Is There A Link Between Food And Eczema?
Food allergies affect about a third of children affected, causing an immediate allergic reaction such as rash, swelling, and abdominal pain – all different to the presentation of eczema. However, food intolerance can inflame your eczema. For example, some fruits can induce the release of histamine in the body, causing temporary itching and redness; this isn’t an allergy but a normal immune response. However, if you are intolerant to that food, a hypersensitive immune response could inflame any eczema symptoms that are present at the time.
So Why Does My Child’s Eczema Get Worse With New Foods?
Parents’ often notice their child’s symptoms get worse when introducing new foods but it is only very rarely due to a true allergy. Eczema tends to reflect stress that the body is facing, and getting used to a new food can be one of those stressors, causing a temporary increase in symptoms. Luckily, this phenomenon often improves after a month or so of new food. We know how important it is to offer young children a wide variety of food, so it’s worth persevering a bit longer to develop that tolerance. Withholding foods unnecessarily may cause more detriment than a temporary worsening of their skin condition.
Nonetheless, if you strongly suspect a food allergy, it is important to consult an allergist for diagnosis and seek further advice about how to offer a nutritionally sound restricted diet.
Are Allergy Tests Reliable?
False positives are common in prick tests on atopic individuals because of the extreme sensitivity of their skin to the disturbance of the pricking method. Blood tests also show many false positives. The unreliability of the results can render allergy testing unhelpful, and even with an accurate positive result, avoidance of these allergens is very difficult, if not impossible. Nevertheless, if you have a genuine allergy and it clearly shows that exposure to the allergen aggravates your eczema, eliminating it from your environment can result in an improvement of your symptoms.
What Are The Treatments For Eczema?
Where possible, reduction of your exposure to trigger factors is always your best line of defense. Subsequently, be prepared that treatment can be required for many months, even years.
First line treatments are almost always topical moisturizers because they’re effective for most patients when used correctly, and they have the fewest side effects. If your eczema is moderate to severe, your treatment plan may also include:
- Medicated topical steroids – creams, ointments, and solutions with an anti-inflammatory action and tar preparations
- Wet wraps – bandages to cover treated areas
- Medications to moderate immune responses – ultimately reducing inflammation
- Antibiotics – for bacterial and fungal infections
- Antihistamines – to relieve itching
- Phototherapy – ultraviolet treatment reserved for severe eczema
- Oral corticosteroids – excellent anti-inflammatories, short term only
- Low concentration antiseptic solutions – can be helpful in managing infected lesions
- Behavioural therapy – to develop mental strategies to break the habit of scratching, which causes grave exacerbation of the condition
- An immunosuppressive agent may be used to treat persistent and severe eczema
Are There Non-Medical Ways Can I Manage My Eczema?
- A brief shower or bath once a day is enough if you have dry skin.
- Use a non-soap cleanser
- Dilute washing powder, use the minimum amount possible, and consider an extra rinse cycle.
- Wear gloves and protective clothing to guard against irritants.
- Only apply specifically prescribed topical solutions to your skin
- Keep the temperature even throughout the house and avoid hot environments
- Cool showers or baths can relieve flare ups
- A residential relocation can be beneficial or detrimental depending on your triggers
- Sun worsens symptoms (photosensitive eczema) in a small percentage of people – minimise exposure
